SALAM is Turning Digital Cardiac Care into Faster Access and Smarter Life-Saving Decisions
Digital health has a communication problem. Too often, it gets told as software, dashboards, platforms, and interfaces. But nobody’s life changes because a platform exists. It changes when care moves differently. That is the real story inside the technical manuals behind the systems SALAM is set to build on: Helis Infarct.NET and Helis Chronical. Strip away the architecture, the workflows and the device integrations, and what emerges is not just a digital stack. It is a model—already tested across more than 4 million people and nearly 200.000 ECG traces a year in Apulia’s emergency telecardiology network—for making cardiac care travel better: from the first contact point to the specialist, from the field to the hub, from fragmented signals to a clinical response that arrives sooner and makes more sense.
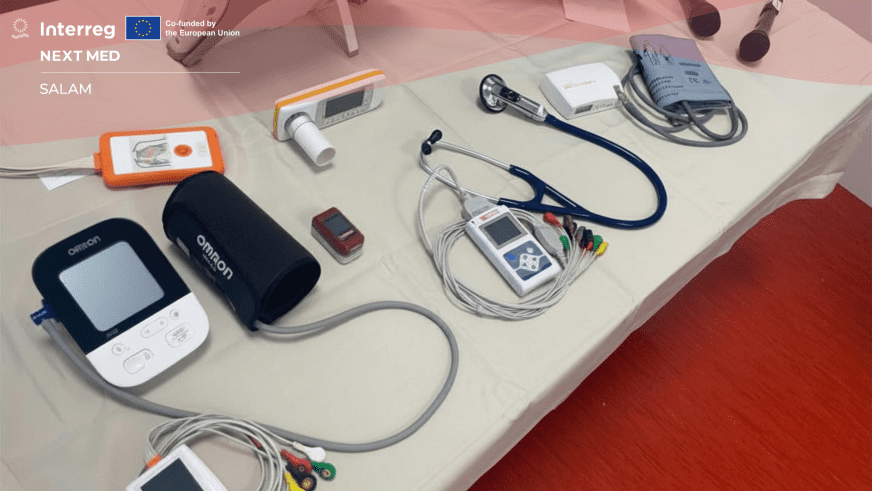
At the centre of the SALAM model is a simple idea: a clinical event should not remain stuck where it begins. Helis Infarct.NET is built for the moment when time matters most. A frontline operator opens a clinical event, assigns a priority, records a 12-lead ECG (an electrocardiogram that reads the heart’s electrical activity from multiple angles) and sends it on for specialist interpretation. On the other side, a doctor in a dedicated control room (the remote clinical centre where cases are reviewed and reported) sees the case arrive, reviews the trace, issues the report and sends it back. The platform tracks the event from start to finish. That may sound procedural. It is not. In practice, it means that an ECG collected outside a specialist setting does not stay there, waiting for the next step to happen. It enters a chain. The first signal becomes a decision point. And that is where the value starts. Not in the fact that the system is digital, but in the fact that it can shorten the distance between suspicion and cardiology.
If Infarct.NET is about urgency, Helis Chronical is about what comes next: continuity, follow-up, coordination, and the slow complexity of staying connected to a patient over time. Its manuals describe a platform built to keep a patient’s case from breaking into fragments. ECGs, heart ultrasound images (echo exams), data from implanted cardiac devices, recorded heart sounds, vital signs (such as blood pressure, oxygen saturation or heart rate), reports from other centres, second opinions and remote consultations can all be brought into the same clinical event. The caregiver or frontline operator can collect and send the data. The specialist can review it through a chronological case log that keeps the whole picture visible as it evolves. That is not just remote monitoring. It is an attempt to stop care from breaking into disconnected pieces. One patient. One event. Multiple inputs. Fewer blind spots.
The wider telecardiology model behind these platforms did not emerge in a vacuum. It builds on an operational experience already developed in Apulia within the Interreg PHASE project (Interreg IPA CBC Italy–Albania–Montenegro 2014–2020), where the regional emergency telecardiology service supported the public ambulance and first-response network known in Italy as the 118 service, served a population of more than 4 million people, and handled nearly 200,000 ECG traces a year from around 400 emergency vehicles and first-aid points. This is not a speculative use case. It is a real system that has already had to work under pressure.

































 Bahrain
Bahrain  Iran
Iran  Iraq
Iraq  Kuwait
Kuwait  Oman
Oman  Qatar
Qatar  Saudi Arabia
Saudi Arabia  Syria
Syria  United Arab Emirates
United Arab Emirates  Yemen
Yemen